📜 Journal Club: High-Flow or Standard Oxygen in Acute Hypoxemic Respiratory Failure
By: BETINA SANTOS TOMAZ, FISIOTERAPEUTA - 03/31/2026 10:43
A study published this month in the New England Journal of Medicine (NEJM), the SOHO trial, brings an important reflection to current clinical practice.
This was a multicenter, randomized clinical trial including more than 1,100 patients with acute hypoxemic respiratory failure, comparing high-flow nasal oxygen (HFNC) versus standard oxygen therapy.
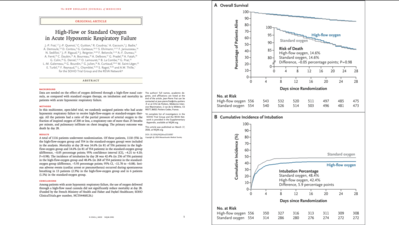
🔍 Key findings
👉 No reduction in 28-day mortality with HFNC (14.6% vs 14.6%)
👉 A modest reduction in intubation (~6%), with borderline confidence intervals
⚠️ Critical question
Are we treating surrogate outcomes rather than clinically meaningful endpoints?
HFNC demonstrated clear physiological benefits:
- ↓ Respiratory rate
- ↓ PaCO₂
- ↑ Comfort and relief of dyspnea
However:
➡️ No impact on mortality
➡️ Time to intubation was essentially identical
➡️ Reduction in intubation was small and borderline
⚖️ Critical interpretation: why no mortality benefit?
Some key hypotheses:
1. 📉 Low event rate
The study was powered to detect a 6% absolute reduction in mortality, but the observed mortality was lower than expected, reducing statistical power.
➡️ Could there be a small but clinically relevant effect?
2. 💉 Improved contemporary care
- High use of corticosteroids
- Protective ventilation strategies
- Better overall supportive care
➡️ The isolated effect of HFNC may have been diluted
3. 🫁 Intubation is not necessarily a “negative” outcome
Reducing intubation does not automatically translate into better prognosis
➡️ Possible explanations:
- HFNC may delay intubation without changing outcomes
- It may select different patients for invasive ventilation
4. ⚠️ Safety signal?
Pneumothorax was numerically higher in the HFNC group (1.8% vs 0.7%)
➡️ Small difference, but biologically plausible
➡️ Possibly related to sustained inspiratory effort (P-SILI?)
🔄 Conflict with previous evidence
This trial directly challenges:
- Frat et al., 2015 (reported mortality benefit)
- COVID-19 era data (suggested reduced intubation rates)
👉 What changed?
- More heterogeneous populations
- Improved global care
- Possible overestimation of prior effects
🧩 What does this change in practice?
This study does not “overturn” HFNC, but it reshapes its role:
✔️ HFNC remains useful for:
- Patient comfort
- Reducing respiratory effort
- Initial respiratory support strategy
❗ But it should NOT be considered:
- A mortality-reducing therapy
- A universally superior strategy
💬 Take-home message
HFNC improves how the patient feels, but not necessarily how the patient evolves.
What are your thoughts on these findings?
Read the full study here: Frat JP, Quenot JP, Guitton C, et al. SOHO Trial Group and the REVA Network. High-Flow or Standard Oxygen in Acute Hypoxemic Respiratory Failure. N Engl J Med. 2026 Mar 17. doi: 10.1056/NEJMoa2516087.
To add an answer on this topic and read the replies...
You must have a valid and active xlung subscription
If you are already a subscriber, please Login at the top of the page, or subscribe now